Cardiovascular Progenitor Cells Derived from Human Embryonic Stem Cells: A Renewable Cell Source for Cardiovascular Studies
Cardiovascular Progenitor Cells Derived from Human Embryonic Stem Cells: A Renewable Cell Source for Cardiovascular Studies
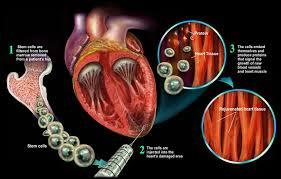
Cardiovascular diseases have long been one of the leading causes of human mortality, and their significance has increased in recent decades. Despite medical advances, conventional therapeutic approaches have limited effectiveness in repairing damage to the heart muscle (myocardium). Consequently, recent research has focused on using cell therapy methods to restore heart muscle function. One of the most valuable cell types in this field is cardiovascular progenitor cells (CPCs) derived from human embryonic stem cells (hESCs). These cells not only hold potential for cell therapy for cardiovascular diseases but also serve as a valuable cell source for studying cardiovascular physiology under laboratory conditions. However, any clinical use of these cells requires the ability to culture them on a large scale.
To develop an efficient culture system using signaling factors that enable the large-scale cultivation of CPCs derived from hESCs, Dr. Hossein Baharvand, Dr. Sara Pehlavan, Dr. Siamak Rezaeiani, Dr. Sadaf Vahdat, and their colleagues at the Royan Institute and Tarbiat Modares University conducted a study. They first differentiated hESCs into cardiac progenitor cells through a four-day process. Subsequently, the resulting cells were maintained and cultured in a simple medium, achieving over six thousand-fold expansion after eight passages. The cells were also successfully cryopreserved for long-term storage.
The results demonstrated that after eight passages, the cells retained their gene and protein expression characteristics as well as their differentiation potential. Additionally, this study, published in the international journal Stem Cell Research & Therapy, showed that cardiac progenitor cells could differentiate into cardiomyocytes, endothelial cells, smooth muscle cells, and fibroblasts with appropriate functionality. Moreover, co-culturing cardiovascular lineage cells derived from cardiac progenitors in collagen led to the formation of cardiac microtissue, highlighting their potential for creating 3D models to study cardiovascular physiology under laboratory conditions.
The study concluded that CPCs derived from hESCs have a commendable ability to proliferate, self-renew, and differentiate into functional cardiovascular lineage cells, maintaining these capabilities through various passages. Therefore, these cells represent a suitable cell source for cardiovascular studies in laboratory settings.



Your Comment :